Connect With Us

Falls Prevention
Elderly Americans are very susceptible to falls as they get older. Everyone experiences decreases in flexibility, balance, strength, and the senses as they age. This correlates to some eye-opening statistics. 1 in 4 Americans aged 65 and older fall each year. An elderly American is being treated for a fall in an emergency room every 11 seconds. In light of these striking statistics, one can see the importance of taking steps to prevent falls.
Finding an exercise program for the elderly is an excellent way to reduce the likelihood of falls. Look for an exercise program that improves strength and balance. Elderly people who live a more sedentary lifestyle, with little physical activity, are at an increased risk of falling. Wearing well-fitted footwear that provides good foot support and cushion will help prevent falls from poorly fitted shoes. Talking to a podiatrist about your susceptibility to falls and about inspecting your prescriptions will help to avoid any medication that could make falls more likely. Due to a decline in the senses among the elderly, having your eyes and hearing checked is recommended.
Around half of all falls occur in the household. Removing tripping hazards in the home and making it more accommodating to older persons can significantly reduce falls. Some notable household changes include increasing lighting around the house, installing grab bars in the shower and bathroom, and making sure the floor is clear of clutter. Other smart options include installing a shower chair, using rubber-bottomed rugs, and placing railings on both sides of stairwells.
Finally, discuss with a doctor and your family about your fear of falling. This will help to increase awareness among the population on the need for fall prevention. A lack of awareness on the matter, and a downplaying of importance are what increase the risks of falling. Following these tips can help to reduce the risk for yourself and your loved ones.
Symptoms and Causes of Ankle Pain
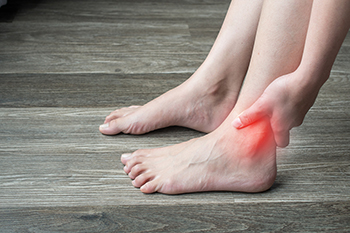
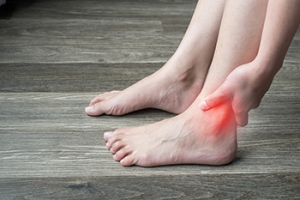
Ankle pain can also result in swelling, and stiffness. While the pain may be sharp, dull, or throbbing, it often intensifies with movement or pressure. Swelling surrounding the ankle can indicate inflammation or injury, leading to visible puffiness and discomfort. Stiffness in the joint can limit mobility, making it difficult to flex or extend the ankle fully. Common causes of ankle pain include sprains, strains, and fractures from trauma or overuse. Conditions like arthritis or tendinitis can also contribute to chronic pain and swelling. A proper diagnosis by a podiatrist is vital to determine the underlying cause and guide appropriate treatment. If you have ankle pain, it is suggested that you contact a podiatrist to determine the cause and offer treatment solutions.
Ankle pain can have many different causes and the pain may potentially be serious. If you have ankle pain, consult with David Mansky, DPM from Mansky Podiatry. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Ankle pain is any condition that causes pain in the ankle. Due to the fact that the ankle consists of tendons, muscles, bones, and ligaments, ankle pain can come from a number of different conditions.
Causes
The most common causes of ankle pain include:
- Types of arthritis (rheumatoid, osteoarthritis, and gout)
- Ankle sprains
- Broken ankles
- Achilles tendinitis
- Achilles tendon rupture
- Stress fractures
- Tarsal tunnel syndrome
- Plantar fasciitis
Symptoms
Symptoms of ankle injury vary based upon the condition. Pain may include general pain and discomfort, swelling, aching, redness, bruising, burning or stabbing sensations, and/or loss of sensation.
Diagnosis
Due to the wide variety of potential causes of ankle pain, podiatrists will utilize a number of different methods to properly diagnose ankle pain. This can include asking for personal and family medical histories and of any recent injuries. Further diagnosis may include sensation tests, a physical examination, and potentially x-rays or other imaging tests.
Treatment
Just as the range of causes varies widely, so do treatments. Some more common treatments are rest, ice packs, keeping pressure off the foot, orthotics and braces, medication for inflammation and pain, and surgery.
If you have any questions, please feel free to contact our office located in Hastings, MI . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Ankle Pain
Pain experienced in the ankle can be caused by a multitude of conditions. While the most common cause is an ankle sprain, other possible problems can include arthritis, gout, ankle instability, an ankle fracture, nerve compression, or tendinitis. In more serious cases, ankle pain can be a sign of improper alignment of the foot or an infection.
Ankle pain can often be accompanied by symptoms such as redness, swelling, stiffness, and warmth in the affected area. Pain can be described differently depending on the condition: short, stabbing pain and a dull ache are some examples. If such symptoms are persistent and do not improve after time, be sure to schedule an appointment with your local podiatrist.
Depending on the condition causing your ankle pain, different treatments may be prescribed by your podiatrist. For ankle sprains, the first step in treatment involves rest, ice, elevation, and compression. Be sure to avoid placing pressure on the ankle, use an ice pack several times a day, and use a compression bandage and elevation to reduce swelling. Other, more serious conditions may require the assistance of certain drugs and medications such as nonsteroidal anti-inflammatory drugs (NSAIDs), physical therapy, or even cortisone injections.
Depending on the severity of your ankle pain and the condition behind it, recovery from ankle pain may take some time.
Consult with your foot and ankle doctor to best determine the cause of your ankle pain and the appropriate treatment.
Arthritis Can Cause Pain in the Feet and Ankles
Exercises Can Improve Foot Health

Engaging in regular exercises focused on the toes, feet, and ankles can significantly enhance foot health and alleviate discomfort. These foot exercises, such as stretching the Achilles tendon, rotating the ankles, and performing heel raises, are beneficial in improving flexibility, strength, and balance. They can be particularly helpful for individuals experiencing foot pain or stiffness. Starting slowly and gradually increasing intensity is advisable, especially for those new to exercise. While these exercises can be done at home, it is wise to consult a podiatrist before beginning any new regimen. A podiatrist can provide personalized advice, ensuring that the exercises you choose are safe and effective for your specific foot condition. This foot doctor can also identify underlying issues that may need professional treatment. If you have problems with your feet, it is suggested that you schedule an appointment with a podiatrist.
Exercising your feet regularly with the proper foot wear is a great way to prevent injuries and build strength. If you have any concerns about your feet, contact David Mansky, DPM from Mansky Podiatry. Our doctor can provide the care you need to keep you pain-free and on your feet.
Exercise for Your Feet
Exercise for your feet can help you gain strength, mobility and flexibility in your feet. They say that strengthening your feet can be just as rewarding as strengthening another part of the body. Your feet are very important, and we often forget about them in our daily tasks. But it is because of our feet that are we able to get going and do what we need to. For those of us fortunate enough to not have any foot problems, it is an important gesture to take care of them to ensure good health in the long run.
Some foot health exercises can include ankle pumps, tip-toeing, toe rises, lifting off the floor doing reps and sets, and flexing the toes. It is best to speak with Our doctor to determine an appropriate regimen for your needs. Everyone’s needs and bodies are different, and the activities required to maintain strength in the feet vary from individual to individual.
Once you get into a routine of doing regular exercise, you may notice a difference in your feet and how strong they may become.
If you have any questions please feel free to contact our office located in Hastings, MI . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Exercise for Your Feet
Foot and ankle pain can be a nuisance in a person’s life, especially if it happens frequently. The best way to prevent this type of pain, is to exercise often. Regular exercise of the foot includes stretching and strength exercises. Stretching exercises can help prevent injuries such as a sprained ankle, while strength exercises can prevent ailments such as plantar fasciitis.
Stretching exercises can help improve flexibility and the foot and ankle’s range of motion. These exercises can certainly help with those who participate in high-energy activities such as sports. Many athletes routinely perform foot and ankle exercises to prevent injuries like sprained ankles, which are common injuries where the tendons in the ankle are over stretched. Strength exercises help develop foot muscles for better support and protection.
Most exercises are simple and can be done at home, either standing or sitting. One chair exercise is called “limber up”. In this exercise, a person would start by sitting down with their feet flat on the floor. Then lift one leg up so the feet are not touching the floor, then rotate your foot clockwise 15-20 times, and 15-20 times counterclockwise. Repeat the same process with the opposite leg. Another sitting exercise helps stretch the back of your heel and requires an exercise band. It begins by looping the band around a heavy piece of furniture, or something stable that will not be moved when the band is tugged or pulled. Then sit directly in front of it, and slide one foot into the loop, so that the band curves around the forefoot. Start by pulling the forefoot back and holding it for 5-10 seconds. Doing this 10-15 times on each foot, will stretch the back of your heel, increasing your flexibility.
Foot exercises that require standing are also just as easy and simple. Referred as the “Achilles Stretch”, this exercise stretches the Achilles tendon, making it more flexible, helping prevent foot, ankle, and leg pain. It begins by first standing and facing the wall, with the arms outstretched and the palms on the wall. Then place one foot behind another keeping the back leg straight, and the forward leg bending at the knee. Make sure both heels are flat on the floor and adjust your stance accordingly. With your hips, lean forward to feel the stretch, you can also adjust the distance from your feet to feel the stretch in various parts of the calf. Make sure to hold the stretch for about 30 seconds and repeat the same process 3 times with each leg. An even easier foot exercise is simply walking on sand. Walking barefoot on sand both strengthens and stretches your feet.
Doing these exercises regularly can help prevent many foot and ankle problems. Other foot exercises can even relieve pain. For example, those affected with plantar fasciitis can simply sit down on a chair, and then place a tennis ball below their affected foot. By rolling the ball under the foot, and increasing or decreasing pressure, pain will be relieved. With any exercise, it is always important to do a small warmup such as walking a few laps around the house to get the blood flowing. If after doing an exercise to relieve pain such as the tennis ball exercise, or are unsure that your execution is correct, be sure to contact a podiatrist for further instruction.
Facts About Athlete’s Foot
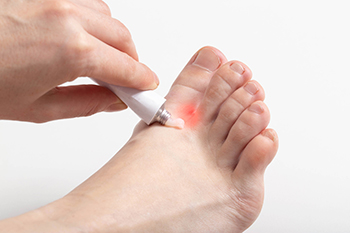
Athlete's foot, medically known as tinea pedis, is a fungal infection that affects the skin on the feet. It commonly manifests in three types, interdigital, moccasin, and vesicular. Interdigital occurs between the toes, moccasin causes scaling on the soles, and vesicular causes fluid-filled blisters. Athlete's foot is caused by fungi that thrive in warm, moist environments, like locker rooms or damp shoes. Symptoms typically include itching, redness, and peeling of the skin, often accompanied by a burning sensation. The infection can spread to other areas of the body if not treated promptly. Maintaining good foot hygiene, keeping feet dry, and wearing breathable footwear can help prevent athlete's foot. If you have an athlete’s foot infection, it is suggested that you promptly visit a podiatrist who can effectively treat this highly contagious condition.
Athlete’s foot is an inconvenient condition that can be easily reduced with the proper treatment. If you have any concerns about your feet and ankles, contact David Mansky, DPM from Mansky Podiatry. Our doctor will treat your foot and ankle needs.
Athlete’s Foot: The Sole Story
Athlete's foot, also known as tinea pedis, can be an extremely contagious foot infection. It is commonly contracted in public changing areas and bathrooms, dormitory style living quarters, around locker rooms and public swimming pools, or anywhere your feet often come into contact with other people.
Solutions to Combat Athlete’s Foot
- Hydrate your feet by using lotion
- Exfoliate
- Buff off nails
- Use of anti-fungal products
- Examine your feet and visit your doctor if any suspicious blisters or cuts develop
Athlete’s foot can cause many irritating symptoms such as dry and flaking skin, itching, and redness. Some more severe symptoms can include bleeding and cracked skin, intense itching and burning, and even pain when walking. In the worst cases, Athlete’s foot can cause blistering as well. Speak to your podiatrist for a better understanding of the different causes of Athlete’s foot, as well as help in determining which treatment options are best for you.
If you have any questions please feel free to contact our office located in Hastings, MI . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Athlete’s Foot
Athlete’s foot, or tinea pedis, is a skin disease caused by a fungal infection. The infection typically occurs between the toes, and the feet are most subject to this disease because shoes best create the warm, dark, and moist environment in which fungus thrives. Other areas that create a similar environment, such as swimming pools, public showers, and locker rooms; can also promote fungi growth.
Symptoms of athlete’s foot include dry skin, itching, scaling, inflammation, and blistering. Sometimes, blisters can evolve into the cracks or breaks in the skin. The exposed tissue can then create pain, swelling, and discharge. The spread of infection can cause itching and burning as well.
While athlete’s foot commonly occurs between the toes, it may also spread to the toenails or soles of the feet. Other parts of the body, such as the groin or underarms, can also become infected if they are touched after the original area of infection is scratched. Aside from physical contact, athlete’s foot can also spread through the contamination of footwear, clothing or bedsheets.
Proper foot hygiene is essential in preventing athlete’s foot. You can prevent the fungus from spreading by frequently washing your feet using soap and water, thoroughly drying the feet between the toes, changing shoes and socks every day to reduce moisture, and ensuring that bathroom and shower floors are disinfected. Other tips include using shower shoes, avoiding walking barefoot in public environments, wearing light and airy shoes, and wearing socks that keep the feet dry.
While treatment for athlete’s foot can involve topical or oral antifungal drugs, mild cases of the infection can be treated by dusting foot powder in shoes and socks. Any treatment used can be supplemented by frequently bathing the feet and drying the toes. If proper foot hygiene and self-care do not ease your case of athlete’s foot, contact your podiatrist. He will determine if the underlying cause of your condition is truly a fungus. If that is the case, a comprehensive treatment plan may be suggested with the inclusion of prescription antifungal medications.
What Is Peripheral Neuropathy?
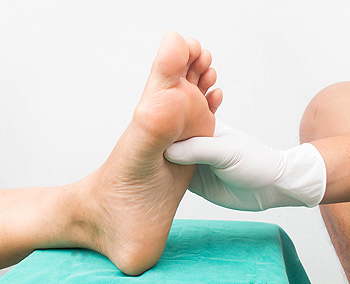
The brain and spinal cord make up the central nervous system, which, under normal circumstances, communicates with other parts of the body through the peripheral nervous system. When nerves within the peripheral nervous system become damaged and interrupt the complex messaging system with the central nervous system, this is known as peripheral neuropathy. Peripheral neuropathy can be caused by diabetes, injury, or autoimmune diseases. Sometimes vascular issues, infections, and certain medications can also cause peripheral neuropathy. This condition can cause stabbing or shooting pain, numbness, cramping, or burning in the feet. It can also result in extreme sensitivity to touch, lack of coordination, or clumsiness. If you are experiencing any of these symptoms, it is suggested that you schedule an appointment with a podiatrist who is adept at diagnosing and managing peripheral neuropathy in the lower extremities.
Neuropathy
Neuropathy can be a potentially serious condition, especially if it is left undiagnosed. If you have any concerns that you may be experiencing nerve loss in your feet, consult with David Mansky, DPM from Mansky Podiatry. Our doctor will assess your condition and provide you with quality foot and ankle treatment for neuropathy.
What Is Neuropathy?
Neuropathy is a condition that leads to damage to the nerves in the body. Peripheral neuropathy, or neuropathy that affects your peripheral nervous system, usually occurs in the feet. Neuropathy can be triggered by a number of different causes. Such causes include diabetes, infections, cancers, disorders, and toxic substances.
Symptoms of Neuropathy Include:
- Numbness
- Sensation loss
- Prickling and tingling sensations
- Throbbing, freezing, burning pains
- Muscle weakness
Those with diabetes are at serious risk due to being unable to feel an ulcer on their feet. Diabetics usually also suffer from poor blood circulation. This can lead to the wound not healing, infections occurring, and the limb may have to be amputated.
Treatment
To treat neuropathy in the foot, podiatrists will first diagnose the cause of the neuropathy. Figuring out the underlying cause of the neuropathy will allow the podiatrist to prescribe the best treatment, whether it be caused by diabetes, toxic substance exposure, infection, etc. If the nerve has not died, then it’s possible that sensation may be able to return to the foot.
Pain medication may be issued for pain. Electrical nerve stimulation can be used to stimulate nerves. If the neuropathy is caused from pressure on the nerves, then surgery may be necessary.
If you have any questions, please feel free to contact our office located in Hastings, MI . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Neuropathy
Neuropathy is a condition in which the nerves in the body become damaged from a number of different illnesses. Nerves from any part of the body, including the foot, can be damaged. There are several forms of neuropathy including peripheral neuropathy, cranial neuropathy, focal neuropathy, and autonomic neuropathy. Furthermore there is also mononeuropathy and polyneuropathy. Mononeuropathies affect one nerve while polyneuropathies affect several nerves. Causes of neuropathy include physical injury, diseases, cancers, infections, diabetes, toxic substances, and disorders. It is peripheral neuropathy that affects the feet.
The symptoms of neuropathy vary greatly and can be minor such as numbness, sensation loss, prickling, and tingling sensations. More painful symptoms include throbbing, burning, freezing, and sharp pains. The most severe symptoms can be muscle weakness/paralysis, problems with coordination, and falling.
Podiatrists rely upon a full medical history and a neurological examination to diagnose peripheral neuropathy in the foot. More tests that may be used include nerve function tests to test nerve damage, blood tests to detect diabetes or vitamin deficiencies. Imaging tests, such as CT or MRI scans, might be used to look for abnormalities, and finally nerve or skin biopsies could also be taken.
Treatment depends upon the causes of neuropathy. If the neuropathy was caused by vitamin deficiency, diabetes, infection, or toxic substances, addressing those conditions can lead to the nerve healing and sensation returning to the area. However if the nerve has died, then sensation may never come back to the area. Pain medication may be prescribed for less serious symptoms. Topical creams may also be tried to bring back sensation. Electrical nerve stimulation may be used for a period of time to stimulate nerves. Physical therapy can strengthen muscle and improve movement. Finally surgery might be necessary if pressure on the nerve is causing the neuropathy.
If you are experiencing sensation loss, numbness, tingling, or burning sensations in your feet, you may be experiencing neuropathy. Be sure to talk to a podiatrist to be diagnosed right away.